Heart
For all its potency, the cone-shaped heart is relatively small, roughly the size of a closed fist, about 12 cm long, 9 cm wide at its widest part and 6 cm thick. Its mass is, on average, 250 g in adult women and 300 g in adult men.
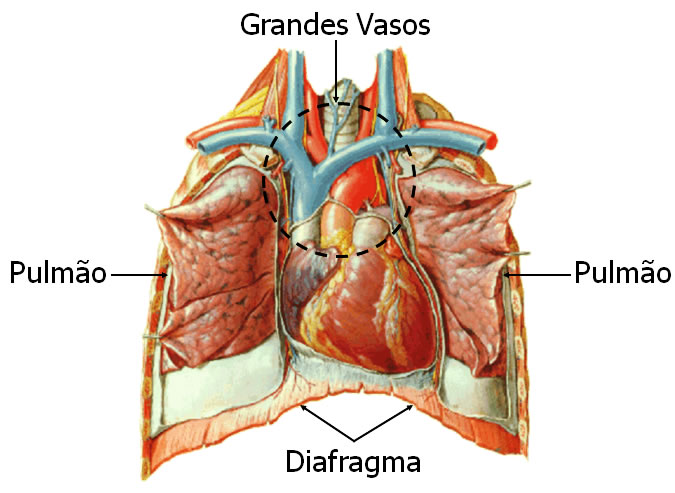
 prayer rests on the diaphragm, near the midline of the thoracic cavity, in the mediastinum, the mass of tissue that extends from the sternum to the spine; and between the linings (pleuras) of the lungs. About 2/3 of the cardiac mass lies to the left of the midline of the body. The position of the heart in the mediastinum is most easily appreciated by examining its extremities, surfaces, and boundaries. The pointed end of the heart is the apex , directed forward, downward, and to the left. The widest portion of the heart, opposite the apex, is the base , directed backwards, upwards, and to the right.
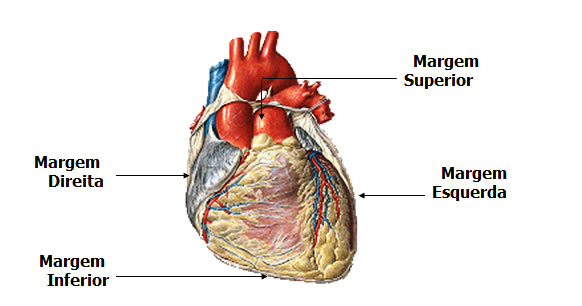
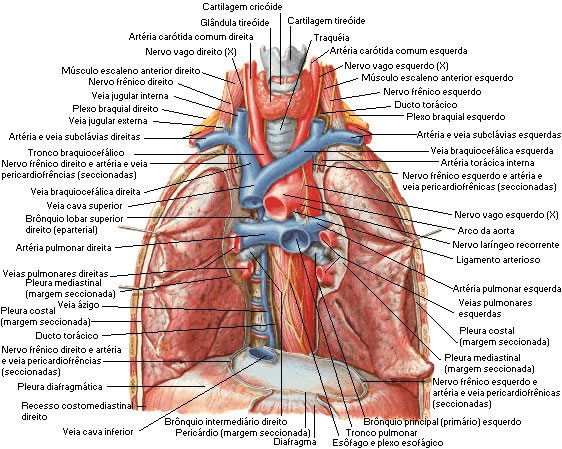
prayer rests on the diaphragm, near the midline of the thoracic cavity, in the mediastinum, the mass of tissue that extends from the sternum to the spine; and between the linings (pleuras) of the lungs. About 2/3 of the cardiac mass lies to the left of the midline of the body. The position of the heart in the mediastinum is most easily appreciated by examining its extremities, surfaces, and boundaries. The pointed end of the heart is the apex , directed forward, downward, and to the left. The widest portion of the heart, opposite the apex, is the base , directed backwards, upwards, and to the right.  Heart Limits : The anterior surface is just below the sternum and ribs. The inferior surface is the part of the heart that, for the most part, rests on the diaphragm, corresponding to the region between the apex and the right approach. The right edge faces the right lung and extends from the inferior surface to the base; the left border, also called the pulmonary border, faces the left lung, extending from the base to the apex. The upper limit is the great vessels of the heart and posteriorly the trachea, esophagus and descending aorta artery.
Heart Limits : The anterior surface is just below the sternum and ribs. The inferior surface is the part of the heart that, for the most part, rests on the diaphragm, corresponding to the region between the apex and the right approach. The right edge faces the right lung and extends from the inferior surface to the base; the left border, also called the pulmonary border, faces the left lung, extending from the base to the apex. The upper limit is the great vessels of the heart and posteriorly the trachea, esophagus and descending aorta artery.
| LIMITS OF THE HEART |
|
| Source: NETTER, Frank H.. Atlas of Human Anatomy. 2nd edition Porto Alegre: Artmed, 2000. |
Cardiac Wall Layers :
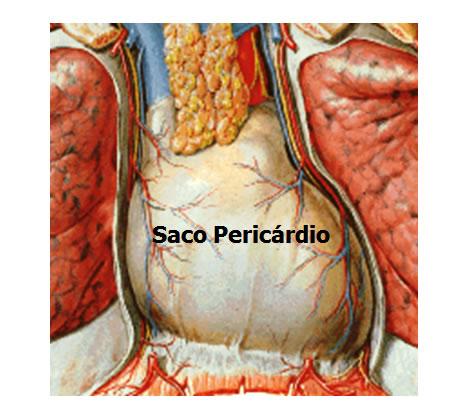
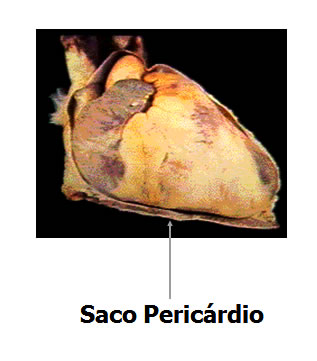
Pericardium: the membrane that lines and protects the heart. It restricts the heart to its position in the mediastinum, while allowing sufficient freedom of movement for vigorous, rapid contractions. The pericardium consists of two main parts: fibrous pericardium and serous pericardium.
The superficial fibrous pericardium is an irregular, dense, tough and inelastic connective tissue. It resembles a bag, which rests on and attaches to the diaphragm.
The deeper serous pericardium is a thinner and more delicate membrane that forms a double layer surrounding the heart. The outermost parietal layer of the serous pericardium is fused to the fibrous pericardium. The innermost visceral layer of the serous pericardium, also called the epicardium, adheres tightly to the surface of the heart.
| PERICARDIAL BAG |
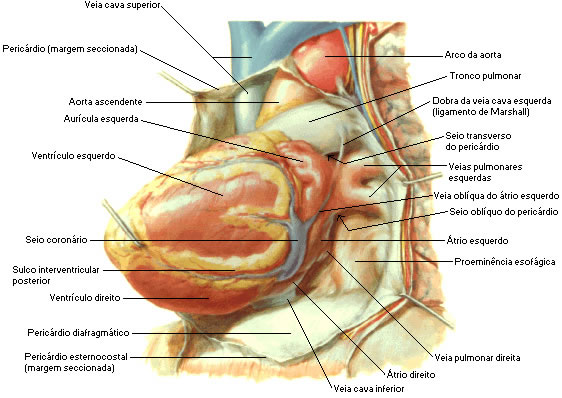
|
| Source: NETTER, Frank H.. Atlas of Human Anatomy. 2nd edition Porto Alegre: Artmed, 2000. |
Myocardium : It is the middle and thickest layer of the heart. It is composed of cardiac striated muscle. It is this type of muscle that allows the heart to contract and therefore push blood, or force it into the blood vessels.
Endocardium : It is the innermost layer of the heart. It is a thin layer of tissue composed of simple squamous epithelium over a layer of connective tissue. The smooth, shiny surface allows blood to flow easily over it. The endocardium also lines the valves and is continuous with the lining of the blood vessels that enter and leave the heart.
EXTERNAL CONFIGURATION :
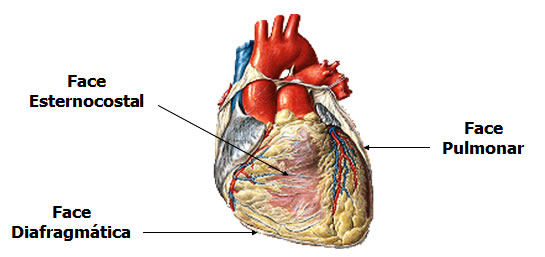
The heart has three faces and four edges:
faces
- Anterior surface (Sternocostal) – Formed mainly by the right ventricle.
- Diaphragmatic Face (Inferior) – Formed mainly by the left ventricle and partially by the right ventricle; it is mainly related to the central tendon of the diaphragm.
- Pulmonary Face (Left) – Formed mainly by the left ventricle; it occupies the cardiac impression of the left lung.
Margin
- Right Margin – Formed by the right atrium and extending between the superior and inferior vena cava.
- Lower Margin – Formed mainly by the right ventricle and, slightly, by the left ventricle.
- Left Margin – Formed mainly by the left ventricle and, slightly, by the left atrium.
- Superior Margin – Formed by the atria and the right and left atria in an anterior view; the ascending aorta and pulmonary trunk emerge from the superior border, and the superior vena cava enters on its right side. Posterior to the aorta and pulmonary trunk and anterior to the superior vena cava, the upper border forms the lower limit of the transverse sinus of the pericardium.
Externally, the atrioventricular ostia correspond to the coronary sulcus, which is occupied by coronary arteries and veins, this sulcus surrounds the heart and is interrupted anteriorly by the aorta arteries and the pulmonary trunk.
The interventricular septum on the anterior surface corresponds to the anterior interventricular sulcus and on the diaphragmatic surface to the posterior interventricular sulcus.
The interventricular sulcus ends inferiorly a few centimeters from the right of the apex of the heart, in correspondence with the notch of the apex of the heart.
The anterior interventricular sulcus is occupied by the anterior interventricular vessels.
This groove is occupied by the posterior interventricular vessels.
The posterior interventricular sulcus starts from the coronary sulcus and descends towards the notch of the apex of the heart.
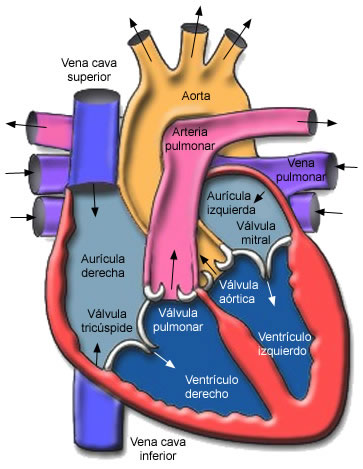
INTERNAL CONFIGURATION :
 The heart has four chambers: two atria and two ventricles. The Atria (the upper chambers) receive blood; Ventricles (lower chambers) pump blood out of the heart
The heart has four chambers: two atria and two ventricles. The Atria (the upper chambers) receive blood; Ventricles (lower chambers) pump blood out of the heart
On the anterior surface of each atrium is a wrinkled, sac-shaped structure called the auricle (similar to a dog's ear).
The right atrium is separated from the left by a thin partition called the interatrial septum; the right ventricle is separated from the left by the interventricular septum.
| INTERNAL CARDIAC CONFIGURATION |
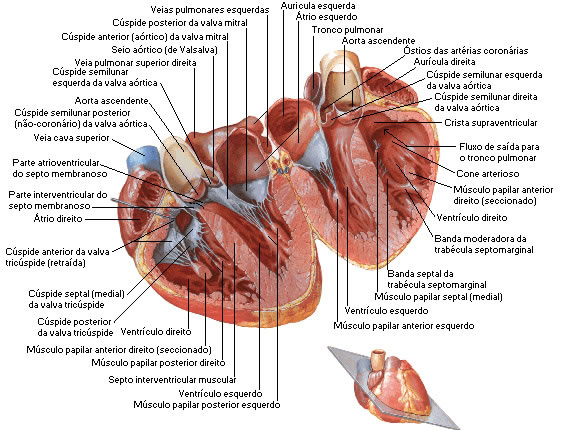 |
| Source: NETTER, Frank H.. Atlas of Human Anatomy. 2nd edition Porto Alegre: Artmed, 2000. |
RIGHT ATRIUM
The right atrium forms the right border of the heart and receives carbon dioxide-rich (venous) blood from three veins: superior vena cava, inferior vena cava, and coronary sinus.
The superior vena cava collects blood from the head and upper part of the body, the inferior receives blood from the lower parts of the body (abdomen and lower limbs) and the coronary sinus receives the blood that nourished the myocardium and carries the blood to the right atrium. .
While the posterior wall of the right atrium is smooth, the anterior wall is rough, due to the presence of muscular crests, called pectinate muscles.
Blood passes from the right atrium to the right ventricle through a valve called the tricuspid (formed by three leaflets – valves or cusps).
On the medial wall of the right atrium, which is constituted by the interatrial septum, we find a depression that is the fossa ovale.
Anteriorly, the right atrium has a pyramidal expansion called the right atrium, which serves to dampen the impulse of blood as it enters the atrium.
The holes where the vena cavas empty are called ostia of the vena cava.
The opening of the coronary sinus is called the coronary sinus ostium and we also find a sheet that prevents blood from returning from the atrium to the coronary sinus which is called the coronary sinus valve.
LEFT ATRIUM
The left atrium is a thin-walled cavity, with smooth anterior and posterior walls, which receives already oxygenated blood; through four pulmonary veins. Blood passes from the left atrium to the left ventricle through the bicuspid (mitral) valve, which has only two cusps.
The left atrium also has a pyramidal expansion called the left atrium.
RIGHT VENTRICLE
The right ventricle forms most of the anterior surface of the heart. Its interior features a series of elevated bundles of cardiac muscle fibers called fleshy trabeculae.
In the right atrioventricular ostium there is a device called the Tricuspid Valve that serves to prevent blood from returning from the ventricle to the right atrium. This valve consists of three membranous, whitish and irregularly triangular laminae, with a base implanted on the edges of the ostium and the apex directed downwards and attached to the walls of the ventricle by means of filaments.
Each blade is called a cusp. We have an anterior, a posterior and a septal cusp.
The apex of the cusps is held by filaments called chordae tendineae , which insert into small fleshy columns called papillary muscles .
The pulmonary trunk valve is also made up of small sheets, but these are arranged in a shell, called semilunar valves (anterior, left and right).
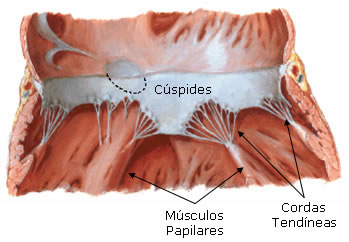
LEFT VENTRICLE
The left ventricle forms the apex of the heart. In the left atrioventricular ostium, we find the left atrioventricular valve, consisting only of two sheets called cusps (anterior and posterior). These valves are called bicuspid. Like the right ventricle, it also has fleshy trabeculae and chordae tendineae, which attach the bicuspid valve cusps to the papillary muscles.
Blood passes from the left atrium to the left ventricle through the left atrioventricular orifice where the Bicuspid (mitral) valve is located. From the left ventricle, the blood goes to the largest artery in the body, the ascending aorta, passing through the Aortic Valve – consisting of three semilunar valves: right, left and posterior. From there, part of the blood flows to the coronary arteries, which branch off from the ascending aorta, carrying blood to the heart wall; the rest of the blood passes into the arch of the aorta and the descending aorta (thoracic aorta and abdominal aorta). Branches of the arch of the aorta and the descending aorta carry blood throughout the body.
The left ventricle receives oxygenated blood from the left atrium. The main function of the left ventricle is to pump blood into the systemic (body) circulation. The left ventricular wall is thicker than the right ventricle. This difference is due to the greater force required to pump blood into the systemic circulation.
| LARGE CARDIAC VESSELS |
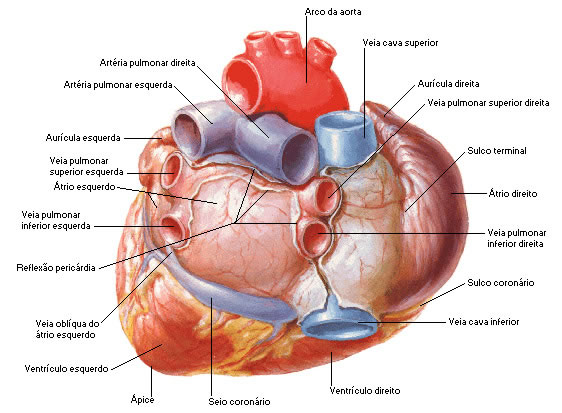 |
| Source: NETTER, Frank H.. Atlas of Human Anatomy. 2nd edition Porto Alegre: Artmed, 2000. |
cardiac cycle
A single cardiac cycle includes all events associated with a heartbeat. In the normal cardiac cycle, the two atria contract, while the two ventricles relax, and vice versa. The term systole designates the phase of contraction; the relaxation phase is called diastole.
When the heart beats, the atria first contract (atrial systole), forcing blood into the ventricles. Once filled, the two ventricles contract (ventricular systole) and force blood out of the heart.r 
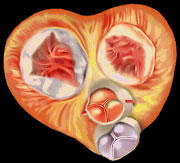

| Valves in Ventricular Diastole | Valve dynamism | Valves in Ventricular Systole |
For the heart to be efficient in its pumping action, it takes more than the rhythmic contraction of its muscle fibers. The direction of blood flow must be guided and controlled, which is achieved by four valves mentioned above: two located between the atrium and ventricle – atrioventricular (tricuspid and bicuspid valves); and two located between the ventricles and the great arteries that carry blood out of the heart – semilunar (pulmonary and aortic valves). Complement: The valves and valves are to prevent this abnormal behavior of the blood, to prevent backflow from occurring they close after the passage of blood.
Systole is the contraction of heart muscle, we have atrial systole that drives blood to the ventricles. Thus, the atrioventricular valves are open to the passage of blood and the pulmonary and aortic valves are closed. In ventricular systole, the atrioventricular valves are closed and the semilunar valves are open to the passage of blood.
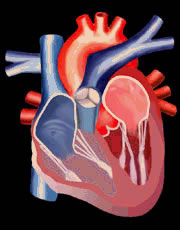
| VENTRICULAR SYSTOLE - ACTION OF ATRIOVENTRICULAR VALVES |
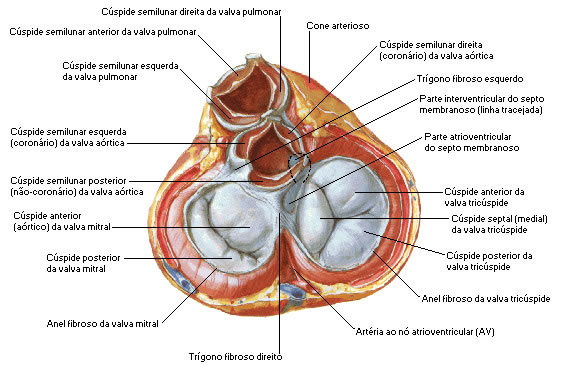 |
| Source: NETTER, Frank H.. Atlas of Human Anatomy. 2nd edition Porto Alegre: Artmed, 2000. |
| VENTRICULAR DIASTOLE - ACTION OF ATRIOVENTRICULAR VALVES |
 |
| Source: NETTER, Frank H.. Atlas of Human Anatomy. 2nd edition Porto Alegre: Artmed, 2000. |
In conclusion, we can say that the cardiac cycle comprises:
1- Atrial systole
2- Ventricular systole
3- Ventricular diastole
Vascularization :
Irrigation of the heart is provided by the coronary arteries and the coronary sinus.
There are two coronary arteries, one right and one left. They have this name because both run through the coronary sulcus and both originate from the aorta artery.
The artery, immediately after its origin, goes to the coronary sulcus, traveling it from right to left, until it anastomoses with the circumflex branch, which is the terminal branch of the left coronary artery that continues this artery, encircling the sulcus. coronary.
The Right Coronary Artery: from the origin of two arteries that will irrigate the right margin and the posterior part of the heart, they are the right marginal artery and the posterior interventricular artery.
The Left Coronary Artery initially passes through a branch behind the pulmonary trunk to reach the coronary sulcus, evident near the apex of the left atrium.
Soon after, it emits an anterior interventricular branch and a circumflex branch that gives rise to the left marginal artery.
On the diaphragmatic surface, the two arteries anastomose, forming a circumflex branch.
Venous blood is collected by several veins that empty into the great vein of the heart, which starts at the apex of the heart, ascends the anterior interventricular sulcus and follows the coronary sulcus from left to right, passing through the diaphragmatic surface, to empty into the atrium. right.
The terminal portion of this vessel, represented by its last 3 cm, forms a dilatation that is called the coronary sinus.
The coronary sinus also receives the middle vein of the heart, which runs from the bottom to the top of the posterior interventricular sulcus and the small vein of the heart that borders the right edge of the heart.
There are also minimal, very small veins, which flow directly into the heart cavities.
Innervation :
The innervation of the heart muscle is in two ways: extrinsic, which comes from nerves outside the heart, and another intrinsic, which constitutes a system only found in the heart and located inside it.
Extrinsic innervation derives from the autonomic nervous system, that is, sympathetic and parasympathetic.
From the sympathetic, the heart receives the sympathetic cardiac nerves, three cervical and four or five thoracic.
The parasympathetic fibers that go to the heart follow the vagus nerve (X cranial nerve), from which parasympathetic cardiac nerves derive, two cervical and one thoracic.
Physiologically, sympathetic speeds up and parasympathetic slows down the heartbeat.
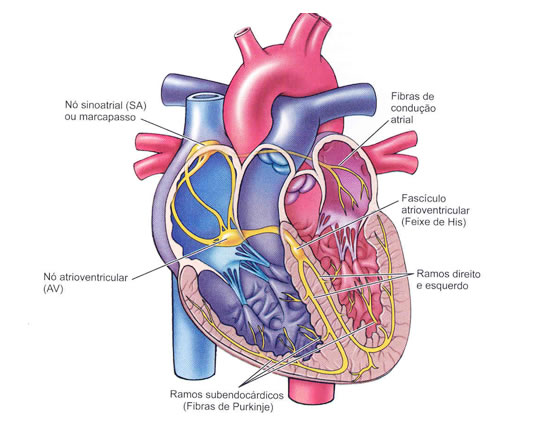
The intrinsic innervation or conduction system of the heart is the reason for the continuous beating of the heart. It is an electrical activity, intrinsic and rhythmic, which originates in a network of specialized cardiac muscle fibers, called auto-rhythmic cells (cardiac pacemakers), because they are self-excitable.
Cardiac excitation begins at the sinoatrial (SA) node, situated in the right atrial wall, inferior to the opening of the superior vena cava. Propagating along the atrial muscle fibers, the action potential reaches the atrioventricular (AV) node, located in the interatrial septum, anterior to the opening of the coronary sinus. From the AV node, the action potential reaches the atrioventricular bundle (bundle of His), which is the only electrical connection between the atria and ventricles. After being conducted along the AV bundle, the action potential enters the right and left branches, which cross the interventricular septum, towards the cardiac apex. Finally, the conducting myofibers (Purkinge fibers) rapidly conduct the action potential, first to the apex of the ventricle and then to the rest of the ventricular myocardium.
| ELECTRICAL HEART SYSTEM |
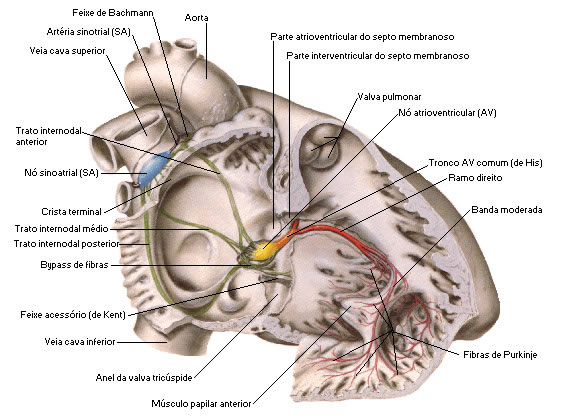 |
| Source: NETTER, Frank H.. Atlas of Human Anatomy. 2nd edition Porto Alegre: Artmed, 2000. |
Diastole is the relaxation of the heart muscle, it is when the ventricles fill with blood, at this moment the atrioventricular valves are open and the semilunar valves are closed.